WITH CONSTRUCTION OF THE FLORINA CANCER CENTER UNDERWAY, SIUH’S NEW CHAIR OF RADIATION ONCOLOGY BRINGS OVER A DECADE OF EXPERIENCE AND CLINICAL EXPERTISE TO THE HOSPITAL’S EVER-EXPANDING DEPARTMENT OF RADIATION MEDICINE
BY AMANDA MCCOY PHOTOS BY AMESSE PHOTOGRAPHY
Of New York City’s five boroughs, Staten Island has the highest prevalence of cancer, and the disease remains the second leading cause of death on the island, behind only heart disease. The leaders of Staten Island University Hospital are responding, investing $45 million into a revolutionary, state-of-the-art cancer center to provide every diagnostic and treatment advantage possible to borough residents. Stretching 40,000 square feet, the Florina Cancer Center brings a sweeping collective of oncologic services under one roof, from research and clinical care to surgery, chemotherapy, immunotherapy, and radiation medicine.
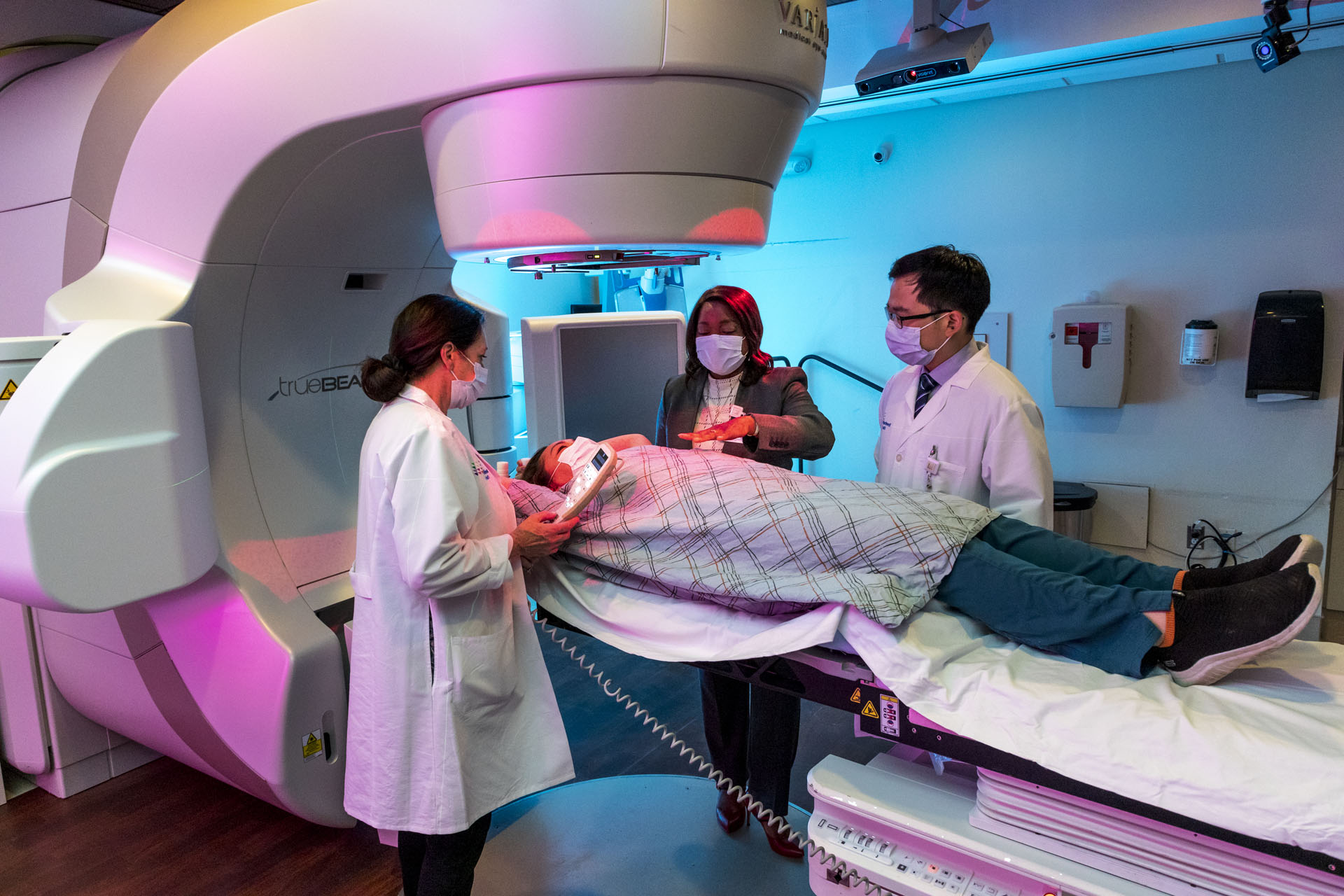
“We are offering incredible multidisciplinary care,” said Chika Madu, MD, chair of radiation oncology at SIUH and a key contributor to the design and technology of the new center. “Across oncology, we are collaborating together to provide the best treatment options possible to cancer patients.”
Dr. Madu was tapped to lead SIUH’s Department of Radiation Medicine in January of this year. Prior to joining the hospital as an attending physician in 2015, the University of Michigan Medical School graduate served as residency program director in the department of radiation medicine at the Lombardi Cancer Center at Georgetown University Hospital. Her vision for the future of the department at SIUH is threefold: focus on patient safety, quality improvement, and establish academic and clinical research as a cornerstone of cancer care.
Radiation therapy a treatment method that uses high doses of radiation to kill cancer cells and shrink tumors is one of the most common types of cancer treatment. In many cases, radiation is employed in tandem with another treatment, such as chemotherapy, surgery, and immunotherapy. The Department of Radiation Medicine at SIUH offers 3-D conventional radiotherapy, intensity modulated radiotherapy (IMRT), image-guided radiotherapy (IGRT), stereotactic radiosurgery (SRS), stereotactic body radiotherapy (SBRT), Brachytherapy, intraoperative radiation therapy (IORT), intravascular brachytherapy (IVBT), and much more.

In the past few years, oncologists have also begun using radiation in combination with pharmaceuticals, a development Dr. Madu called exciting. This new therapy follows a targeted approach to treating certain types of cancer, delivering radiation via pharmaceuticals that bind to the cancer cells directly. Because these radiopharmaceuticals are intended to specifically target diseased cells while leaving healthy tissue untouched, the treatment can reduce systemic side effects.
“The technology and imaging equipment we use is innovative and state of the art, but what’s exciting about the new center is not just the building itself, but the talent we have there. Our ability to collaborate with our colleagues surgical oncologists, medical oncologists, hematology oncologists – means that we can come up with the best course of action for our patients using evidencebased medicine. The department also recently recruited Dr. Daniel Ma, a radiation oncologist, who joined the department in August 2022. We are fully integrated within the Northwell Health system and maintain the same quality of care and standards across all of radiation medicine within Northwell. All of our physician leaders have virtual conferences every day. We review upcoming patient treatment plans across our different sites, so that when a treatment plan is devised, the patient can be assured that all eyes have been on his or her case.”
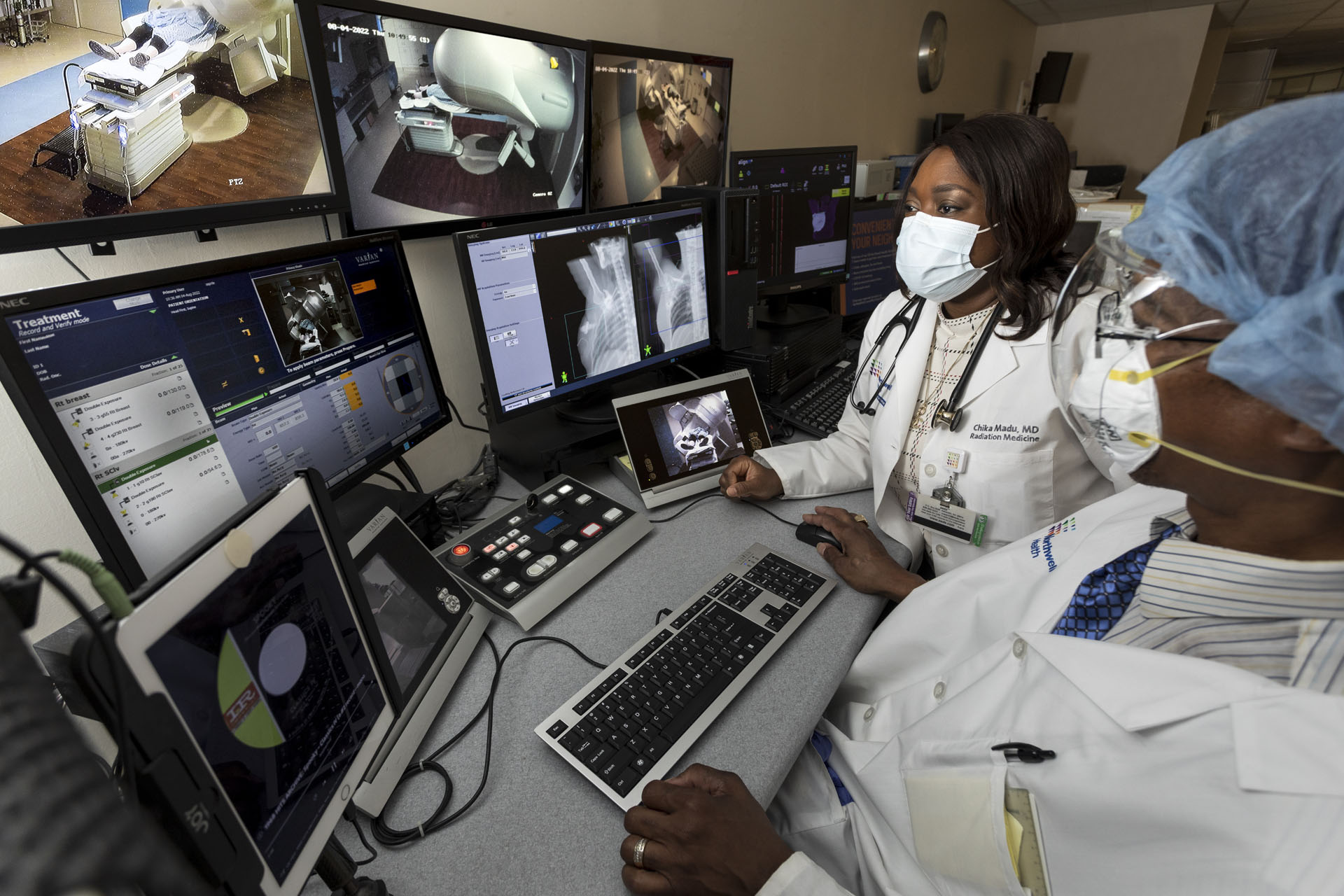
Research has long been a focus of Dr. Madu’s practice. She currently serves as a co-lead in the American Society for Radiation Oncology’s CHEDI commit – tee, an advocacy group aimed at eliminating barriers to minority enrollment into clinical trials. She’s also working to expand access to clinical trials for Staten Islanders, so they can participate in leading-edge therapies close to home without the need to travel into Manhattan or beyond.
“The research department within Northwell Health is completely integrated as well,” she said. “Most of the studies open in the main hub, and as a satellite, we have the opportunity to attach ourselves to those studies, as well as open brand new clinical trials here. We want Staten Island residents to know that they don’t have to truck into the city to participate in these types of trials.”
One example of an upcoming clinical trial studies the effects of delivering intraoperative radiation at the time of surgery for recurrent GBM, an aggressive brain tumor that is notoriously difficult to cure.

“Oftentimes after initial treatment, patients with GBM have to come back for additional surgery. For patients who are fit to undergo another surgical procedure, we can use a specialized machine to deliver radiation at the time of surgery. We look forward to offering this opportunity to patients in Staten Island.”
The introduction of AI, noted Dr. Madu, has also been a significant game changer in her field. “We have software that will auto contour. We give the machine the patient’s anatomy, then it finds the liver, heart, spinal cord, etc. and maps out all those organs for us. We can take a look and make modifications if needed, but it helps us complete treatment planning much more quickly.”
Leading-edge technology is paramount in delivering the latest care, said Dr. Madu, but she was quick to point out that the staff at SIUH is what truly makes the difference. The Department of Radiation Medicine at SIUH has received the prestigious North Star 90 Award three of the last four years, which is Northwell Health’s highest honor.
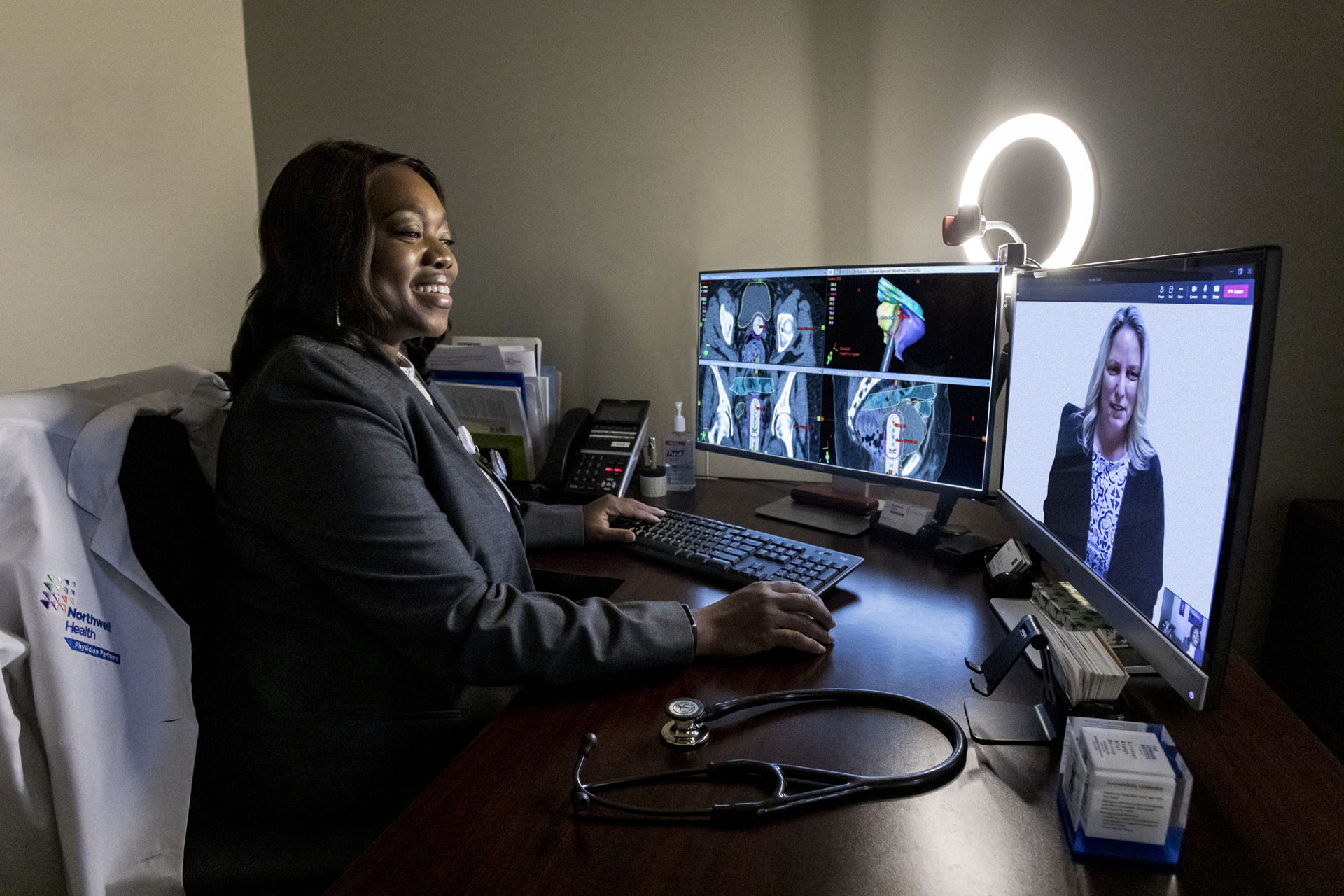
“My team are my people,” said Dr. Madu. “They will care for you like you are their family, and patients feel that love. We have patients that will say they have no appetite, the only food they could possibly eat is ravioli, and my staff will then go home and personally cook them ravioli. The patients and their families put their trust in us, and we take that to heart.”
This interpersonal experience, said Dr. Madu, is what initially prompted her to pursue a career in radiation oncology.
“No one ever wakes up and plans for a cancer diagnosis,” she continued. “When that happens to a person, it changes their world. What we do is help patients get through one of the most difficult times in their life. Our goal is curative, to make that cancer go away and not come back, which is very fulfilling. But palliative care is also important. When there’s no cure available but someone is in pain because of a tumor, we are able to provide palliative radiation to ease the pain and improve that patient’s quality of life in their final months. It’s heartwarming to know that we are able to help.”
SIUH Department of Radiation Medicine
siuh.northwell.edu/cancer-institute/radiation-medicine
