INNOVATIONS WITHIN SIUH’S CARDIOLOGY PROGRAM ALLOW DOCTORS TO DELIVER CRITICAL CARE TO PATIENTS ONCE CONSIDERED TOO HIGH RISK
BY JESSICA JONES-GORMAN • PHOTOS BY AMESSE PHOTOGRAPHY
Over the past two years, the programmatic advances within the Cardiology program at Staten Island University Hospital (SIUH) have been numerous, poising the department as one of the most advanced in the region. Upon introducing several new interventional therapies in 2019, the hospital is delivering critical care to patients who were previously considered too high risk for traditional treatments. And in the next several months, the radiation oncology and interventional cardiology teams at SIUH will partner to deliver a new form of coronary care here in our borough, bringing even more life-saving innovations to the residents of Staten Island.
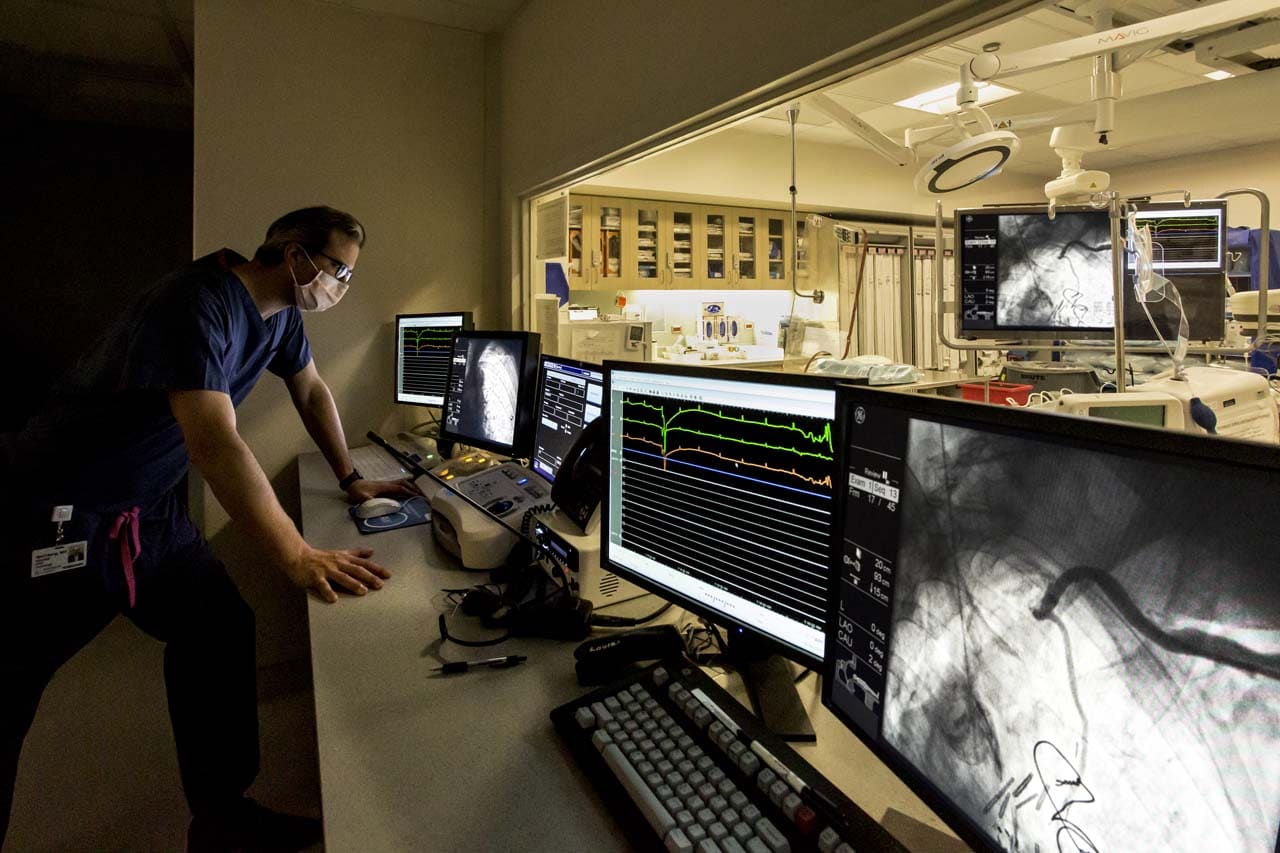
“Staten Island University Hospital’s Interventional Cardiology and Electrophysiology programs are extremely strong and continually growing,” noted Dr. Mitchell D. Weinberg, chair of cardiology at SIUH. “Employing minimally invasive coronary interventions and utilizing new technology that allows doctors to treat complex lesions in the coronary arteries, our team is working to provide the best in coronary care. It is truly an exciting time for this hospital and for the field of cardiology in general.”
Identifying the Cardiac Catheterization Lab’s Complex Total Occlusion Program (CTO) as “groundbreaking,” Dr. Weinberg detailed how he and his staff handle these complex occlusions, which are aimed at healing patients who are experiencing chronic chest pain despite medications.
“Patients are rigorously selected via a multidisciplinary team including cardiologists, cardiothoracic surgeons, and radiologists. Once a patient is identified as a CTO candidate, a detailed plan of care is created using advanced imaging to map the blockage. Technology such as imaging software, diamond tipped burr catheters, and lasers are used to access and dissolve the hardened plaque that is causing an arterial blockage. The procedure is minimally invasive, can be performed with moderate sedation, and has a short recovery period.”

The Complex High Risk Percutaneous Coronary Intervention Program (or CHIP), designed for those with complex anatomy, multiple co-morbidities (multiple chronic conditions), or poor hemodynamics (blood flow), also allows interventional cardiologists to provide potentially life-saving care to patients who could not have withstood an invasive cardiac procedure.
“Similar to the CTO program, each patient is carefully screened by a multidisciplinary team to determine suitability for a CHIP procedure,” the doctor said. “During the procedure, a left ventricular support device called Impella may be inserted to maintain the patient’s hemodynamic status. The Impella device pumps oxygenated blood from the left side of the patient’s heart to the rest of the body, decreasing the work load on the patient’s heart muscle.”
According to the cardiologist, both the CTO and CHIP programs are revolutionary.

Dr. Weinberg earned his bachelor and medical degrees from the University of Pennsylvania. He completed his internal medicine residency at Columbia Presbyterian Hospital, his cardiology and interventional cardiology fellowships at Mount Sinai Hospital, and an advanced fellowship in vascular medicine and vascular intervention at Massachusetts General Hospital. He recently obtained an MBA from the Zarb School of Business at Hofstra University.
Prior to SIUH, Dr. Weinberg served as director of peripheral vascular intervention at North Shore University Hospital, expanding programs across Long Island. His responsibilities were extended to Lenox Hill Hospital and the surrounding Western region of the health system, where he advanced vascular medicine and intervention broadly. He was recruited by SIUH to serve as chair of cardiology in May. Aiming to engage the Island’s population and spread the word of SIUH’s advanced cardiac care to every corner of the borough, Dr. Weinberg is currently focused on growing the hospital’s burgeoning services.
“In addition to growing our heart failure and vascular intervention departments, we are concentrating on cardiac imaging, bringing a host of technology into diagnostics. We currently have a robust cardiac CT program and a strong cardiac MRI program, and we will continue to develop those even further.”
In the next several years, the cardiologist expects to see continued growth in the hospital’s structural heart program.

“We’ve been performing minimally invasive aortic valve replacement surgeries for close to three years, and this year we’re adding a mitral valve minimally invasive treatment. The program is a beautifully combined effort between our cardiology and cardiothoracic departments. Once that is in place, there is nothing in the structural heart side that our group of doctors will not deliver.”
Dr. Weinberg says the program is emblematic of what the hospital is trying to achieve on the Island.
“We are combining and reorganizing our talent in order to provide Staten Island patients with something uniquely profound,” he said.
And starting in 2020, SIUH’s Departments of Radiation Oncology and Interventional Cardiology will partner together to provide coronary brachytherapy.
“Brachytherapy is a procedure recommended for patients with coronary artery disease (CAD) who have had stents placed and have developed scar tissue within the stent leading to blockage,” the doctor explained.
During the procedure, a catheter is placed within the blocked stent and a radioactive isotope is introduced by the radiation oncologist via the catheter. A very low dose of intracoronary radiation is delivered to the patient by a radiation oncologist, inhibiting regrowth of the scar tissue within the stent.
“The basis of this treatment is to prevent restenosis plaque,” Dr. Weinberg said, detailing the re-accumulation of plaque within an artery that has been previously treated with a balloon or stent. “The procedure itself is another example of combining disciplines to deliver advanced care.”
In the field of electrophysiology, Dr. Marcin Kowalski has taken the lead at SIUH to advance the treatment of cardiac arrhythmias.

“As an internationally recognized researcher and content expert, Dr. Kowalski was chosen as the first electrophysiologist in the United States to use the newest generation cryoballoon to treat atrial fibrillation,” the hospital noted. “In early 2019, Dr. Kowalski traveled to Japan to help introduce this cutting-edge technology. Many of the techniques Dr. Kowalski has developed in cryoablation at SIUH are now used at hospitals globally.”
Dr. Kowalski was also chosen as one of six electrophysiologists in the United States to pilot the latest mapping system that will be used to identify and treat arrhythmias. is technology will reduce the amount of radiation exposure to patients, while still providing precise anatomical information to the electrophysiologist during ablations. Once FDA approved, SIUH says the technology will become the standard of care for patients suffering from arrhythmias.
According to Dr. Weinberg, it’s just one of the many innovative therapies that SIUH will focus on implementing in the near future.
“In the future we are going to place new emphasis on preventative therapies,” the doctor concluded. “Building upon our excellent procedural, interventional, and structural heart programs, we plan on not only delivering advanced therapies with ease but also emphasizing preventative measures that will protect our patients’ health.”
SIUH Department of Cardiology Division of Interventional Cardiology & Vascular Intervention
501 Seaview
Avenue, Suite 300 / 718.663.7000 /
siuh.northwell.edu

