HOW THE MAIMONIDES HEART RHYTHM CENTER PROVIDES BROOKLYNITES WITH THE LATEST IN INNOVATIVE 21ST-CENTURY CARDIAC CARE
BY JESSICA JONES-GORMAN PHOTOS © AMESSÉ PHOTOGRAPHY
Over the past several years, Maimonides Medical Center has become a leading institution in the tri-state region in the care of arrhythmias by applying the most advanced technologies and procedures to treat patients. Having performed over 200 hybrid atrial fibrillation (A-fib) ablations a procedure combining expertise of both cardiothoracic surgeons and electrophysiologists by freezing or burning cardiac tissue that is sending incorrect electrical signals to cause an abnormal heart rhythm Maimonides Heart & Vascular Institute specialists offer several innovative therapies at its Heart Rhythm Center. Doctors there say the program is only continuing to grow.

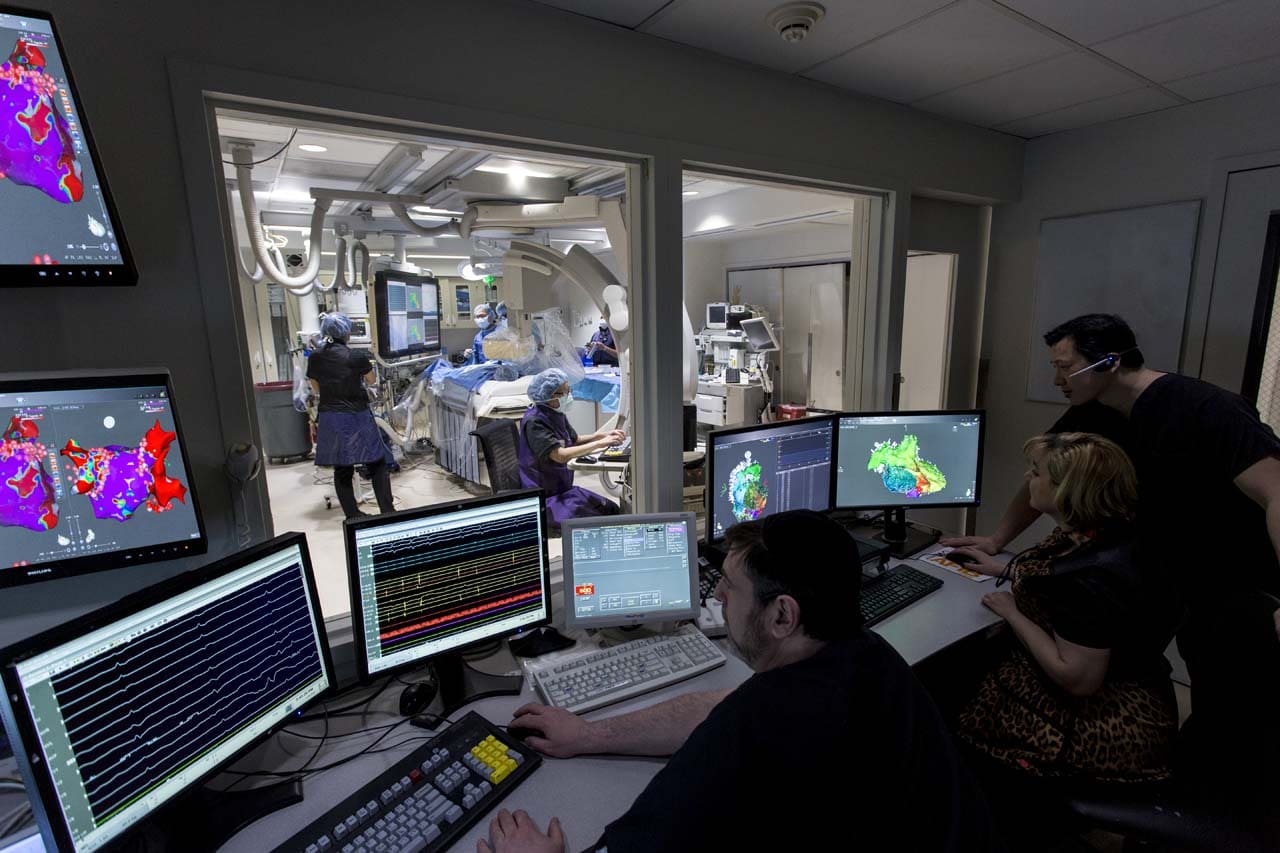
“Technology has come a long way in society, and so has our ability to map arrhythmias in the body,” noted Dr. Yisachar Greenberg, Director of Cardiac Electrophysiology at Maimonides, detailing the evolution of intraoperative mapping techniques in cardiac arrhythmia surgery, which allow physicians to see the critical components of an arrhythmia circuit. “We have three mapping systems available, each providing great detail about ablation options and each allowing us to map very complex arrhythmias in a rapid fashion.”
Dr. Greenberg, who earned his degree from SUNY Downstate before completing his residency at Long Island Jewish Medical Center and a fellowship at Yale New Haven Hospital, has been with Maimonides for 23 years and is credited with helping launch its Heart Rhythm Center.
Dr. Greenberg, who earned his degree from SUNY Downstate before completing his residency at Long Island Jewish Medical Center and a fellowship at Yale New Haven Hospital, has been with Maimonides for 23 years and is credited with helping launch its Heart Rhythm Center.

The Electrophysiology team, in conjunction with Dr. Israel Jacobowitz, the Cardiothoracic Surgeon with whom it performs hybrid A-fib ablations, have had notable success with this innovative procedure: 85 percent of patients remained in normal sinus rhythm (NSR) at their one-year follow-up appointment. The Heart Rhythm Center has also actively participated in numerous NIH and FDA clinical research trials over more than 20 years, and the hospital’s cardiology research team works closely with the Heart Rhythm team to provide the most innovative therapies. Dr. Greenberg reported that his team treats approximately 7,000 outpatients each year.
“We see a lot of patients, but still offer personalized care,” he said. “Our goal is to be actively involved in each and every case, whether we’re implanting a device or monitoring remotely while the patient is at home.”
Dr. Felix Yang, who serves as Associate Director of Cardiac Electrophysiology and Director of the Lead Extraction Service at Maimonides, agreed.
“The volume of complex procedures and device extractions has certainly increased since I’ve been here,” noted Dr. Yang, who has been handling lead extractions and A-fib ablations for the hospital for the past eight years. “But as the amount of cases increases, the technology to treat them continues to improve, allowing us as physicians to be more efficacious in our procedures.”
Dr. Yang categorized the electrophysiology procedures at Maimonides into two large groups: Device implantation and arrhythmia treatment.

“Device implantation encompasses approximately one half of our patient population, who either have too slow of a heartbeat and need a pacemaker or those at risk for dangerously fast heart rhythms who require an implantable defibrillator,” Dr. Yang explained. “The other half of our patients with arrhythmias are often treated with medications or an ablation procedure to burn or freeze an area of the heart, destroying the tissue from which abnormal electrical signals cause arrhythmias.
The Maimonides Heart Rhythm team now provides patients with incredibly small and lightweight pacemakers. These next-generation heart assist devices do not require attached wires inside a patient’s body. The procedure to implant these devices does not require incisions rather, a small puncture in the groin or leg allows electrophysiologists to thread the pacemaker up to the heart with minimal discomfort and rapid recovery time. For patients with these new devices, there is no external evidence of a pacemaker in place.
The mapping procedures Dr. Greenberg referenced in which diagnostic catheters are threaded through blood vessels and used to map the heart’s electrical signals are an integral part of this procedure.
“Ablation is an evolving landscape, and new tools and technologies are being developed rapidly to treat a number of different arrhythmias,” said Dr. Yang, who completed his medical school, internship, and residency training at Cornell. He completed a fellowship in Cardiovascular Medicine at Beth Israel Medical Center, and a second fellowship in Cardiac Electrophysiology at Montefiore Medical Center. Dr. Yang was inspired to pursue this profession by his father.
“My father was a cardiologist, and I decided to follow in his footsteps. I found cardiology to be the most interesting field of study and practice for me,” he said.
During his training, Dr. Yang focused on electrophysiology, because the specialty allowed him to immediately solve patients’ conditions.
“I found that to be very gratifying,” he explained, adding that the field has developed rapidly since that training.
“iPhones, Fitbits, and other personal devices are sort of changing the way we diagnose,” Dr. Yang said. “Patients are coming in more frequently because watches are picking up an irregular heartbeat. The ability of these devices to pick up on that has definitely caused an increase in the number of people we see. That type of technology and advancement is actually saving lives.”
In the future, Dr. Greenberg expects to see a number of advances in ablation therapy, allowing physicians to approach arrhythmias even more effectively, and with less risk to the tissue adjacent to the heart. He said that devices like pacemakers might also be powered by the energy of the heartbeat itself, not batteries. All such advances are a testimony to the power of technology.
“Medicine has become so enamored with this subspecialty,” Dr. Greenberg concluded. “People are now recognizing the presence of arrhythmia and rhythms that were not treatable before, but are now. It’s a wonderful time for this area of medicine.”
The Maimonides Heart & Vascular Institute
4802 Tenth Avenue / 888.MMC.DOCS/
nycHeart.org
