A KEY PLAYER IN THE HOSPITAL’S RAPIDLY EXPANDING CANCER PROGRAM, SIUH’S DIRECTOR OF HEAD AND NECK ONCOLOGY DISCUSSES CLINICAL BREAKTHROUGHS, GROUNDBREAKING TRIALS, AND WHY THE PATIENT RELATIONSHIP REMAINS HIS CAREER’S BIGGEST REWARD
BY AMANDA MCCOY • PHOTOS BY AMESSE PHOTOGRAPHY

In January 2020, as a part of an ambitious plan to revolutionize cancer care in the borough, Staten Island University Hospital officially broke ground on the Florina Cancer Center, a 40,000-squarefoot, state-of-the-art facility that would bring a sweeping collective of cutting-edge oncologic services under the same roof. It signified the massive investment the hospital was putting into expanding its cancer program. Michael Blasco, MD, a decorated head and neck surgical oncologist with specialized training in reconstruction, was eager to be a part of it.
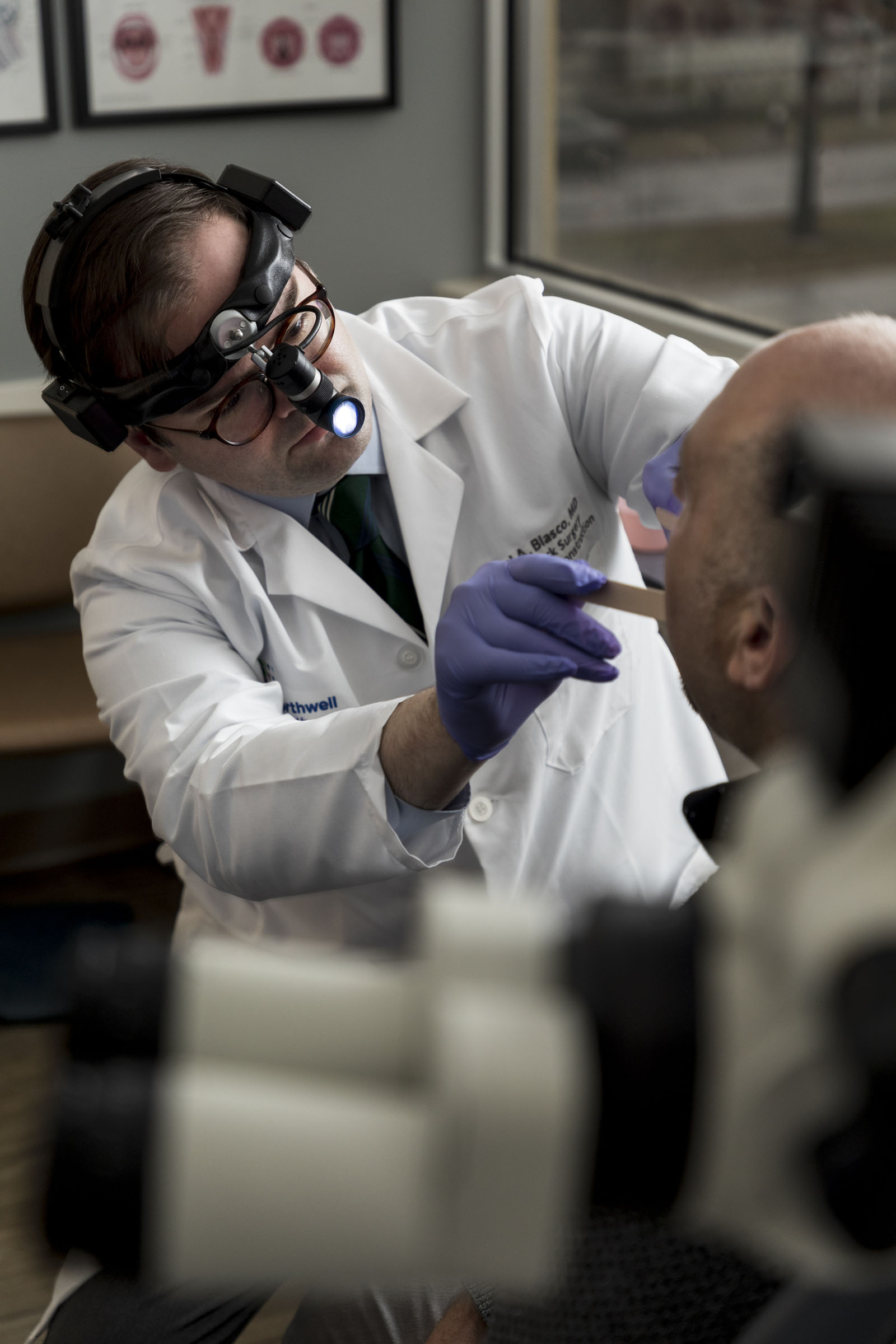
“It’s an exciting time to be at SIUH,” noted Dr. Blasco, director of head and neck oncology and reconstruction. “The investment Northwell Health [SIUH’s parent network] is making in the cancer program is substantial. We are not only increasing the number of patients we see but working to constantly improve the quality of care. One thing that appealed to me about the hospital is its commitment to the community. We are providing world-class, complex, high-level care while taking care of our population. It’s fulfilling to join an organization that’s dedicated to growing and improving.”
A Chicago native and graduate of the University of Illinois College of Medicine, Dr. Blasco joined SIUH after completing a fellowship in head and neck surgical oncology with the University of Toronto, where he pursued a special focus on reconstruction. He treats a wide range of conditions that involve the head and neck, from benign thyroid growths and small melanomas to complex cancers of the voice box or throat. “It’s a perfect place to be in medicine because I get the opportunity to form lasting relationships with my patients and help them through one of the most difficult times of their life.”
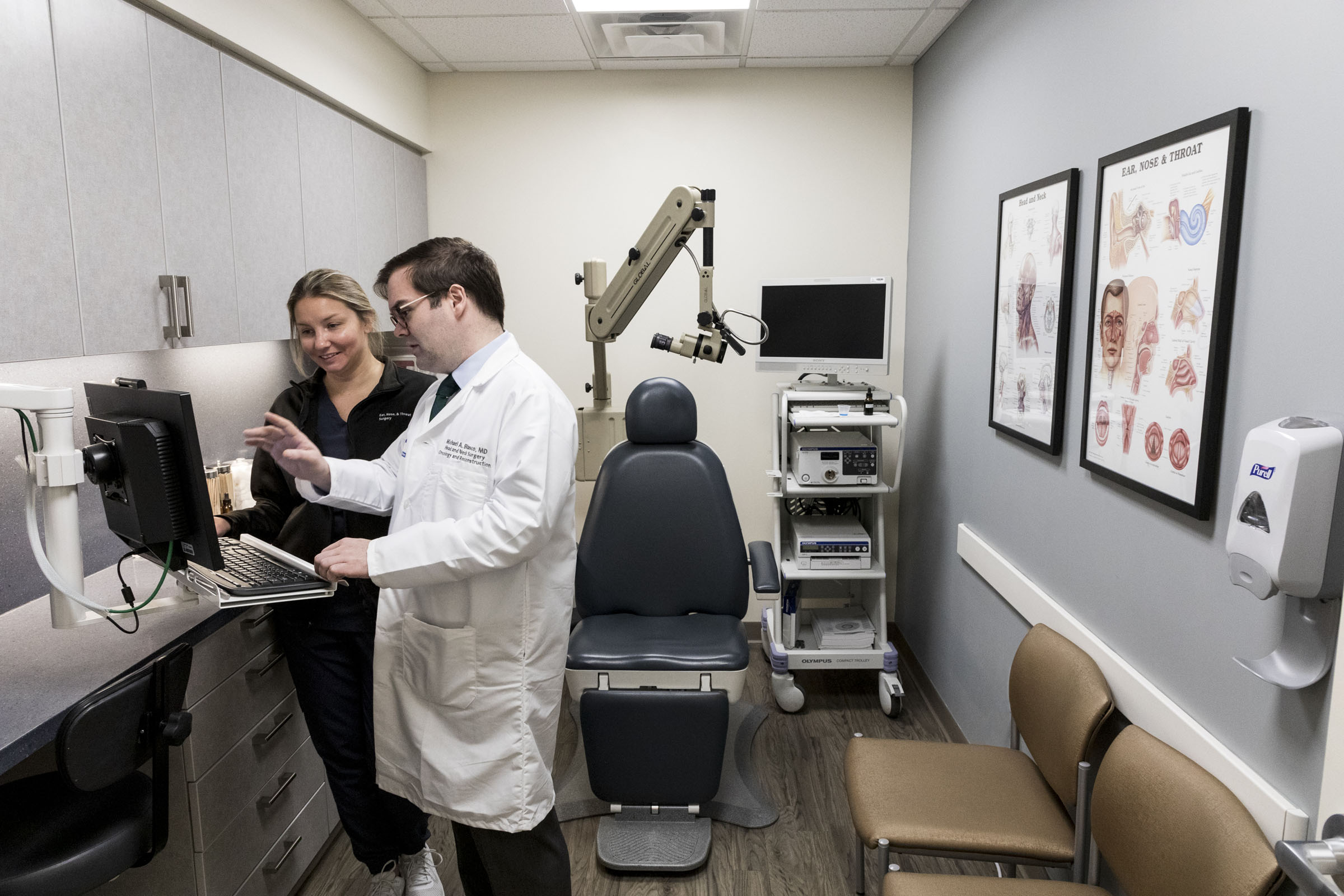
Accounting for approximately 4% of all new cancer diagnoses in the U.S. (per data from the National Cancer Institute), head and neck cancers can form in the mouth, throat, larynx, swallowing passage, nasal passage, and salivary glands. While tobacco or excessive alcohol use is often the cause, Dr. Blasco noted a lesser-known but rapidly rising risk factor is the human papillomavirus (HPV), which now accounts for more than half of all oropharyngeal diagnoses (cancers of the throat, base of tongue, tonsils, and back of mouth). The good news, the doctor pointed out, is this type of cancer can be prevented with the HPV vaccine.
Describing head and neck oncology as highly multidisciplinary, Dr. Blasco routinely collaborates with imaging specialists, radiation oncologists, medical oncologists, speech and language pathologists, and other surgeons to determine the best course of treatment for his patients. With numerous groundbreaking advancements in robotic surgery over the past decade, patients have access to more minimally invasive options than ever before. Dr. Blasco specializes in transoral robotic-assisted surgery, for example, to remove certain types of tumors through the mouth that once required a large incision along the jaw or throat. During the procedure, precision robotic arms are equipped with high-resolution cameras, allowing the doctor to access small, hard-to-reach places of the mouth or throat.

Reconstruction is also an important element of Dr. Blasco’s practice. Even if a surgery is successful and the tumor is fully eradicated, the patient’s journey might not be over. Removing large or complex tumors can leave large gaps in the tissue of the mouth or disrupt a person’s ability to swallow or speak. “Removing the tumor is only one part of the story,” explained Dr. Blasco. “Our goal is to return the patient to full function and restore their quality of life. That’s where reconstruction comes in. Over the last 20 years, we’ve revolutionized what we can do as doctors to make sure patients have the best long-term quality of life following a complex operation.”
One such area is micro vascular reconstruction surgery, a procedure that uses bone, muscle, and/or skin (along with their associated blood vessels) from other parts of the body to rebuild areas that were damaged by the tumor. “We can completely restore form and function after complex tumor removal surgeries,” added Dr. Blasco.

Though cancer remains the second leading cause of death in the U.S. (behind heart disease), the mortality rate has been steadily declining for years as early detection methods improve and treatments become less invasive. To continue pushing the needle of progress forward, Dr. Blasco has participated in several clinical trials throughout his career. He’s currently investigating new ways to treat early-stage oral cavity cancer through sentinel lymph node biopsy, a procedure that uses an imaging agent (like a dye) to identify and then remove only cancerous lymph nodes. “The goal is to limit the amount of radical surgery a patients needs to undergo,” he said.
It was during his residency in otolaryngology at Wayne State University in Detroit when Dr. Blasco came to fully appreciate the deep, long-term bonds that could form between oncologists and their patients. In describing his approach to patient care, Dr. Blasco said he believes in a shared decision-making model, one that presents patients with all the information they need to make their own informed decisions about their healthcare. For him, that’s why the doctor-patient experience is so important it needs to be based on trust.

“It’s rare to get the opportunity to build a lifelong relationship with a patient,” he said. “The partnerships you form when you’re helping people navigate one of the most di cult parts of their life is rewarding. You’re not just involved in the treatment, but in helping them get back to living the lives they want to live. I’m continually amazed by the patients I take care of, to witness the level of strength, courage, and tenacity they demonstrate, adapting to cancer treatment and coming out stronger on the other side.”


